When Surgery Meant Death: How C-Sections Went From Desperate Last Resort to Everyday Procedure
Picture this: It's 1850, and a woman in labor is struggling. The baby won't come naturally, and both mother and child are in grave danger. The local doctor faces an impossible choice—attempt a cesarean section, which will almost certainly kill the mother, or watch both patients die.
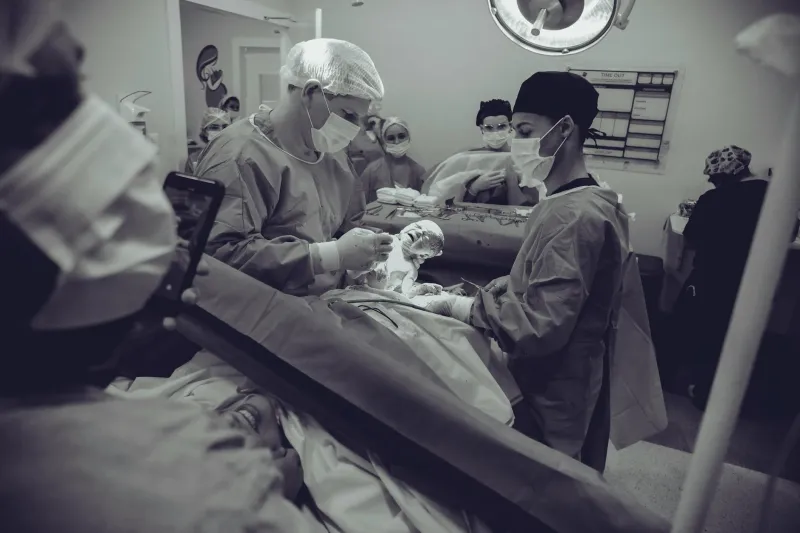
Fast-forward to today, and that same scenario plays out very differently. The mother gets wheeled into a sterile operating room, receives a spinal block, and within 30 minutes, she's holding her healthy baby. She'll likely go home in two days, with nothing more than a small scar as evidence of major surgery.
This transformation—from death sentence to routine procedure—represents one of medicine's most dramatic reversals. Yet most Americans have no idea just how remarkable this change really is.
The Grim Reality of Early Cesareans
For most of human history, cesarean sections were performed only on dying or dead mothers. The name itself comes from the Roman law Lex Caesarea, which required the procedure to save babies when mothers died in childbirth. The idea of both mother and child surviving was virtually unthinkable.
Even into the 1800s, maternal mortality from C-sections hovered near 100%. Infection was almost inevitable. Anesthesia didn't exist until the mid-1800s, meaning women endured the surgery fully conscious. Most hospitals were breeding grounds for deadly bacteria, and surgeons operated without gloves, often moving from autopsy tables directly to operating rooms.
Dr. James Barry performed one of the first successful C-sections where both mother and baby survived in 1826 in South Africa. It was so extraordinary that medical journals documented it as a near-miracle. In America, the first successful cesarean wasn't recorded until 1827, and such cases remained newsworthy events well into the 20th century.
The Slow Climb to Safety
The transformation didn't happen overnight. It took nearly a century of medical advances working together to make cesarean delivery viable.
Antiseptic surgery, introduced by Joseph Lister in the 1860s, began reducing infection rates. The development of anesthesia meant women could undergo surgery without dying from shock and pain. Blood transfusions, perfected during World War I, addressed the massive blood loss that often accompanied the procedure.
But even by 1950, C-section rates in America hovered around 3-4% of births. The procedure was still reserved for genuine emergencies—cases where natural delivery would likely kill mother or baby. Most women delivered at home with midwives, and hospitals were places you went to die, not to have babies.
The Modern Revolution
Today's reality would astound those early physicians. Nearly 32% of American babies are born via C-section—that's over 1.2 million procedures annually, making it one of the most frequently performed surgeries in the country.
The maternal mortality rate for cesarean delivery has plummeted to roughly 0.02%—a 5,000-fold improvement from the 1800s. Modern techniques include regional anesthesia that keeps mothers awake and alert, antibiotics that prevent infection, and surgical methods that allow for faster healing and shorter hospital stays.
What changed? Everything. Fetal monitoring lets doctors detect problems before they become life-threatening. Ultrasound technology reveals complications early. Better surgical techniques, from improved suturing methods to refined incision placement, have made the operation safer and recovery faster.
The Complications of Success
But this medical triumph has created new questions that would have puzzled doctors from earlier eras: When is surgery the right choice?
In 1970, the World Health Organization suggested that C-section rates above 10-15% indicated overuse. Today, rates vary wildly across America—from 23% in some states to nearly 40% in others. Some hospitals perform cesareans in over half of all deliveries.
Factors driving the increase include older mothers (who face higher risks), multiple births from fertility treatments, and legal concerns that make doctors more likely to recommend surgery rather than risk complications during natural delivery. Some women actively choose C-sections for scheduling convenience or to avoid labor pain.
Critics argue we've swung too far—that a procedure once reserved for life-or-death situations has become routine for convenience. Supporters point out that modern C-sections are so safe that the risk-benefit calculation has fundamentally changed.
A Complete Reversal
The story of cesarean delivery represents something remarkable in medical history: a complete reversal of outcomes. A procedure that once guaranteed death now saves lives routinely. Surgery that required desperate circumstances is now planned weeks in advance.
Your great-great-grandmother would have viewed a C-section as a death sentence. Your daughter might schedule one like a dentist appointment.
This shift reflects more than just medical progress—it shows how dramatically our relationship with surgery, childbirth, and medical intervention has changed. We've moved from an era where any surgical intervention was terrifying to one where major surgery has become so routine that we debate whether we're doing too much of it.
The next time you hear about someone having a C-section, remember: you're witnessing the end result of one of medicine's most dramatic transformations, a procedure that went from certain death to everyday occurrence in just over a century.